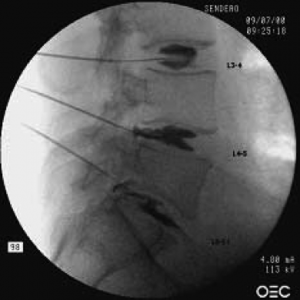
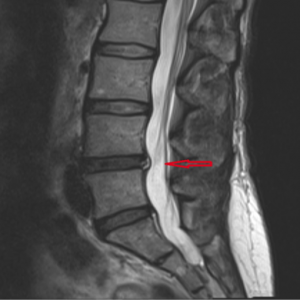
As you get older, the structure of your spine changes gradually, especially around the intervertebral discs. These changes can result in degenerative disc disease, when pain in the back occurs because of vertebral discs that have been damaged or have started to prematurely deteriorate. When degenerative disc disease first occurs, the patient might not experience many symptoms. As the problems progress though, the patient will generally suffer severe back pain that requires the intervention of a spine doctor and can even spread into the leg. There are a number of physical activities that can make the chronic pain of degenerative disc disease worse, including:
- Sitting
- Bending forward
- Coughing
- Sneezing
- Standing
- Walking
This is because of the pressure these physical activities place on the discs. Patients suffering from degenerative disc disease may require the intervention of a spine doctor to stop or reverse the deterioration as well as pain management techniques to help them cope with symptoms.