This content was medically reviewed by Baher S. Yanni, MD, on September 16th, 2021.
Everyone will deal with back pain at one point or another in their lives, and when you think about it, it is not really a surprise. Our spines have a staggering number of moving parts, all in close proximity to the brain’s main connection to the rest of our bodies. The spine is a mass of bone, cartilage, nerves and other tissue, and that means there is no space for any of the pieces to get out of alignment or wear down. In a perfect world, every part of everyone’s spine would stay in place. However, that is not the case, and when anything in the spine is troubled, you feel it. The discomfort can be strong enough to shrink your abilities, activities, and therefore your life. That is why we are here.
When we chose to dedicate our precious time to studying and healing the spine, we chose a great subject because there is always more to learn. It does not matter what you’re doing; your spine is part of it. With all the ways we tend to contort, twist, push and pull our bodies, it is actually amazing that our spines do as well as they do for as long as they do. When the spine is not happy, nobody is happy, and that is why we are so passionate about discovering ways to relieve the spine so our patients can dive back into life. Even better, we continue to be dedicated to providing non-invasive solutions because fast recovery and fewer complications are very important.
In our years of treating back issues of all kinds, we have noticed that there is a good deal of ambiguity around herniated discs and spinal stenosis. People do not fully understand the differences between the two, which makes it difficult to pursue the correct treatment from professionals. Not only that, misunderstanding what is happening in your back affects the way you treat it each day, which may lead to you making the problem worse while thinking you are making it better. Today, we want to explore herniated discs and spinal stenosis in order to bring some clarity to them. Read on!
Herniated Discs 101
Your spine has 33 individual bones that all need to work together peacefully. When they fail to do this, you experience serious pain, nerve issues and even paralysis.
When you have a bunch bones that need to come together and form joints, there are some special extra parts required to make it work. One such crucial part is a disc. It acts as a pillow between bones, absorbing shocks and preventing the bones from touching or pinching the nerves that run between them. It can take quite a beating because it features a very tough exterior made of concentric sheets of collagen fibers. Its core has loose fibers suspended in a mucoprotein gel, allowing it to flex, compress and move with the bones around it while staying in place. You have 23 such discs between the vertebrae in your back, working right now to keep you comfortable and functional.
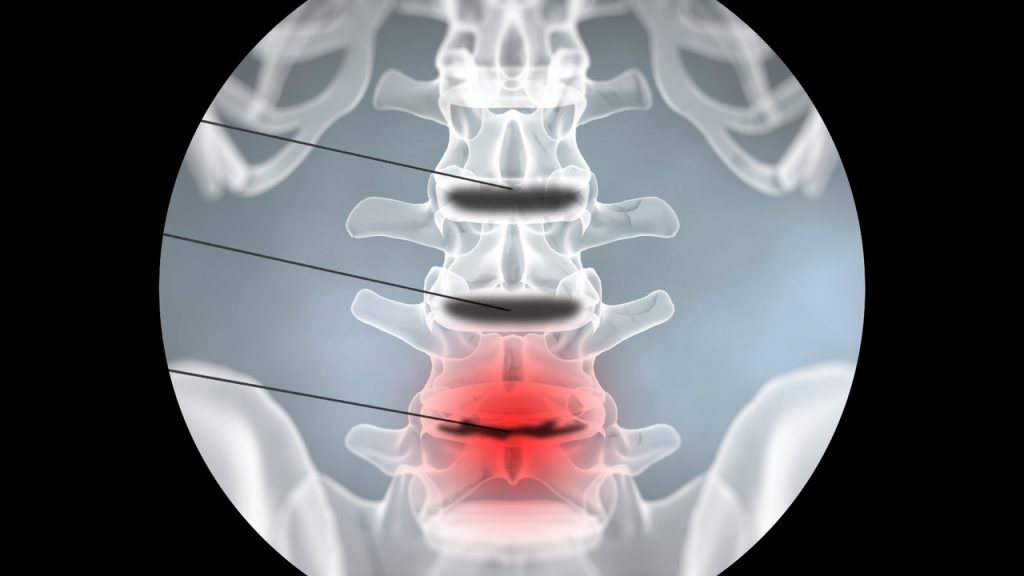
So what does it mean when a disc is “herniated?” Well, as a general term, “herniated” means “to protrude abnormally from an enclosed cavity or from the body.” When a disc gets old or takes just a bit too much of a beating, its hard shell gets damaged, and the soft nucleus starts to seep through weak points. The disc can no longer fulfill its function and generally will start to protrude into its surroundings. That is why you will hear a herniated disc also called “slipped” or “ruptured.”
As we mentioned before, there is no room in the spine for any part to be out of alignment. When a disc stops padding a joint and instead bulges out into the surrounding space, it does not matter what it hits; it is bad. Herniated discs press against nerves, important tissues and impede your spine’s ability to distribute weight correctly.
Herniated Disc Symptoms
A variety of symptoms can crop up when you have a herniated disc. Most of the time, this issue occurs in the lower back or lumbar spine, but it can also occur in your neck or cervical spine. If you’re not sure if you have a herniated disc, the most common signs and symptoms include:
- Buttocks, thigh and calf pain
- Possible foot pain
- Shoulder and arm pain
- Shooting pain if you move or cough
If nerves are affected, you may experience pain, numbness, tingling, sciatica, muscle spasms or leg weakness. Muscle weakness may cause stumbling and it can even impair your ability to hold or lift items. If the disc presses against your cauda equina nerve bundle, you can lose control of your entire lower body, leading to incontinence and loss of feeling. This is one of the most serious symptoms of a slipped disc and should be addressed immediately by emergency medical personnel.
In some cases, you may have a herniated disc without experiencing any symptoms at all. In these instances, you may not know you have one unless it shows up on spinal images.
How Do We Treat Herniated Discs?
The good news here is that herniated discs don’t generally require surgery. As long as you are not experiencing the drastic symptoms we just mentioned, the first treatment for a herniated disc is to get the inflammation down and give the body a chance to help itself out. Pain medications and anti-inflammatories will become your best friends, and you will probably need hot and cold compresses, special exercises, and even a steroid injection to bring the inflammation down. Our experts will do everything they can to provide you with the tools you need to help your body.
Herniated Disc Surgery
If the pain will not subside after pursuing these conservative treatment options, we have more good news for you: you don’t need to undergo a serious operation. Instead, we can perform an endoscopic discectomy, which uses a tiny incision about one-fourth of an inch long to carefully access the troubled disc with an endoscope and camera. This operation is minimally invasive and allows the surgeon to understand just what is going on and does not even require general anesthesia.
As opposed to traditional spinal surgery, this procedure allows patients to spend less time in the hospital and offers decreased healing time. Because it causes less trauma to the spine’s muscles and soft tissue, most patients require less time to heal and only need minimal pain medication.
Spinal Stenosis 101
While a hernia involves something busting outward into space it does not belong, “stenosis” is almost the complete opposite. The term “stenosis” refers to the narrowing of a body channel in a way that is not normal. When the channel of bone that shields your spinal cord shrinks down, it is called “spinal stenosis,” and it can show up anywhere along the spine. Some people are born with it, but for many people, it starts to happen as they get older and their spines deteriorate.
Spinal Stenosis Symptoms
When the spinal cord starts to get compressed by the bones that are supposed to protect it, you will feel it. Many people experience numbness, weakness and pins-and-needles when stenosis occurs in their lumbar (lower) spine. If stenosis occurs in your mid-back, you’ll feel pain in your internal organs, back and ribs. If stenosis shows up in your upper back, it can lead to paralysis. That is why we recommend that anyone feeling the symptoms of spinal stenosis get medical treatment as soon as possible. It is better to have cried wolf and be okay than assume the problem isn’t serious and have to live with difficult issues.
Some general spinal stenosis symptoms to look out for occur in three categories:
- Pain Symptoms: Patients with spinal stenosis often experience pain in their legs, thighs, backs of the legs, neck and buttocks.
- Muscular Symptoms: You could experience difficulty walking or keeping your balance. It may also cause cramping or muscle weakness.
- Sensory Symptoms: Along with the above-mentioned numbness, weakness and pins-and-needles sensations, patients also tend to lose some touch sensations.
Patients can experience these symptoms at any time, but they often feel more intense when going from a sitting to a standing position or exercising. Bending forward or sitting often relieves the symptoms associated with spinal stenosis.
In some cases, patients have spinal stenosis and don’t realize it. In these cases, the only way to determine if you have the condition is through spinal images.
How to Treat Spinal Stenosis and Surgical Intervention
As with most spinal issues, the first things to do is try to calm things down with muscle relaxers, painkillers, compresses, massage, and steroid injections. We always pursue conservative treatment options before exploring some of the minimally invasive procedures offered at Spine INA.
If the pain persists, surgical intervention may be required. However, most of our operations are minimally invasive with a shorter recovery time and minimal hospitalization. We can perform an endoscopic foraminoplasty, a procedure that only requires a half-inch incision and conscious sedation. This is an incredible alternative to other spinal stenosis treatment that requires large incisions and all the risks that come with general anesthesia.
How Can You Prevent Spinal Stenosis and Herniated Discs?
The best cure is prevention, and the team at the Spine INA team does all we can to help people avoid herniated discs and spinal stenosis in the first place. It’s important to understand that your back wears out as you get older, and the more you do to maintain a durable spine, the longer it will last. Here are some great things you can do:
- Stay physically active. This helps your spine stay flexible and strengthens your back and abdominal muscles, which gives your spine extra support.
- Manage your weight. The more weight you carry, the more strain your spine has to manage, and the sooner it will have troubles.
- Play smart. High impact sports like football, hockey and gymnastics commonly cause spinal injuries, so it is a good idea to pursue activities that don’t slam your spine, like yoga, swimming and walking.
Contact Spine INA to Find the Cause of Your Back Pain
There are many ways the spine can start to break down or have trouble, and we are fortunate to live in an age where we can actually understand what is going on underneath the skin. That being said, many of the patients we meet with in New Jersey are practically at the ends of their ropes. Determining the cause of back pain can be a very confusing, contradictory and frustrating journey for patients, who can end up bouncing from specialist to specialist in an exhausting quest for relief.
At the Spine INA, we are equipped to get to the root of the problem because all of our processes are designed to carefully, thoroughly and effectively identify and treat back issues. We settle for nothing less than absolute clarity. When you turn to us for treatment, you get access to a world-class team of professionals who not only understand the spine in all of its complexity but also have a passion for preserving your health and comfort. If you feel like your back issue cannot be solved, it’s time to give us a call. Make an appointment with us in New Jersey today!










With a lateral stenosis impinging on the s1 nerve caused by herniated disc which treatments do you normally do?
Hi Tony! To discuss treatment options such as this, we would love for you to give us a call or fill out a contact form! That way we can best tailor a response 🙂 Thanks!
I found out this week that i was treated for stenosis of cervical neck. When i actually had 4 herniated and bulging disks which physical therapist didnt know.would that cause me problems 3 years later as im about crippled
Hi Paul! We are so sorry to hear about the challenges you have had to face. In order to discuss your medical status, please fill out a contact form on our site or give us a call!
I want to know if im crippled worse today because dr sent orders to physical therapy after i was involved in a whiplash.she sent instructions for stenosis but forgot to put rest of report on the order stating about my 4 herniated neckdisks
I have spine stenosis and at s1 s2. I m a gym trainer. And only income person. Please tell how could I rec. Myself. Can it possible to be cured by ashan.
Hey there! Please give us a call and we can discuss! Thanks.
Good Evening,
I have 2 bulging herniated disks and spinal stenosis in lower back. I also have Congestive Heart failer with coronary artery disease. I have 5 stents already in my heart. My Question is would surgery for my back be safe?
Hey there John! We’d be happy to chat about this with you and help to determine that – can you give us a call? Thanks!
Can u contact me when u can i had questions about spinal stenosis and heirnated disk thanks
Hi Gerry! Please feel free to give us a call and we are happy to answer any questions!
If one has central canal stenosis of the vertebra (likely congenital), is one then more vulnerable to slight slippage or bulges of discs into the canal (than one who does not already have central stenosis).
Thanks-
Jon
Hey Jon! In order to help provide some insight there, we’d like to learn more on the context of this question! Please give us a call 🙂 Thanks so much!